CrashSavers Trauma/Tourniquet
| Part of | CrashSavers Trauma |
|---|
Almost a third of civilian mortality from trauma is preventable, and 64% are from extremity hemorrhage.[1] Early, effective tourniquet application is a hemorrhage control technique known to substantially reduce mortality.[2][3] However, untrained personnel have been found to have unacceptably high rates of tourniquet failure when asked to apply a tourniquet using only the package instructions.[4] A recent randomized controlled trial identified that even after targeted tourniquet training, military recruits still had high rates of tourniquet failure.[5] As such, the Hartford Consensus of 2015 recommended medical and non-medical personnel learn how to apply a tourniquet.[6]
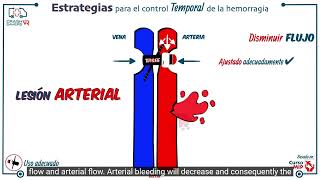
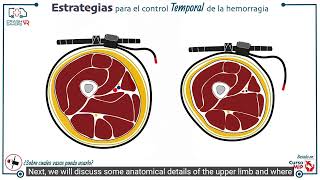
A tourniquet is a tight, band-like device intended to compress a bleeding vessel enough so that blood flow stops completely. Often, these devices function by compressing soft vessels against surrounding hard bone. When profuse arterial bleeding cannot be controlled with pressure or packing, or when there are multiple sites of bleeding, a tourniquet can be beneficial. The tourniquet is ideally placed 2-3 inches above the location of bleeding, and at least 100 mmHg pressure over systolic blood pressure is needed to be effective.[7]
How it Works
[edit | edit source]Many types of ready-made tourniquets exist, but in a setting where one is not readily accessible, a tourniquet can be created using fabric and a rigid stick to provide adequate compression. Our Simulator model will allow providers to learn how to correctly apply tourniquets for hemorrhage control.
References
[edit | edit source]- ↑ Davis JS, Satahoo SS, Butler FK, Dermer H, Naranjo D, Julien K, Van Haren RM, Namias N, Blackbourne LH, Schulman CI. An analysis of prehospital deaths: Who can we save? J Trauma Acute Care Surg. 2014 Aug;77(2):213-8. doi: 10.1097/TA.0000000000000292. PMID: 25058244.
- ↑ Kragh JF Jr, Walters TJ, Baer DG, Fox CJ, Wade CE, Salinas J, Holcomb JB. Survival with emergency tourniquet use to stop bleeding in major limb trauma. Ann Surg. 2009 Jan;249(1):1-7. doi: 10.1097/SLA.0b013e31818842ba. PMID: 19106667.
- ↑ Kragh JF Jr, O'Neill ML, Walters TJ, Dubick MA, Baer DG, Wade CE, Holcomb JB, Blackbourne LH. The military emergency tourniquet program's lessons learned with devices and designs. Mil Med. 2011 Oct;176(10):1144-52. doi: 10.7205/milmed-d-11-00114. PMID: 22128650.
- ↑ Dennis A, Bajani F, Schlanser V, Tatebe LC, Impens A, Ivkovic K, Li A, Pickett T, Butler C, Kaminsky M, Messer T, Starr F, Mis J, Bokhari F. Missing expectations: Windlass tourniquet use without formal training yields poor results. J Trauma Acute Care Surg. 2019 Nov;87(5):1096-1103. doi: 10.1097/TA.0000000000002431. PMID: 31274827.
- ↑ Tsur AM, Binyamin Y, Koren L, Ohayon S, Thompson P, Glassberg E. High Tourniquet Failure Rates Among Non-Medical Personnel Do Not Improve with Tourniquet Training, Including Combat Stress Inoculation: A Randomized Controlled Trial. Prehosp Disaster Med. 2019 Jun;34(3):282-287. doi: 10.1017/S1049023X19004266. Epub 2019 May 2. PMID: 31043185.
- ↑ https://www.facs.org/about-acs/hartford-consensus
- ↑ Tejwani NC, Immerman I, Achan P, Egol KA, McLaurin T. Tourniquet cuff pressure: The gulf between science and practice. J Trauma. 2006 Dec;61(6):1415-8. doi: 10.1097/01.ta.0000226159.84194.34. PMID: 16983305.
| Authors | CrashSavers |
|---|---|
| License | CC-BY-SA-4.0 |
| Organizations | Global Surgical Training Challenge |
| Cite as | CrashSavers (2021–2026). "CrashSavers Trauma/Tourniquet". Appropedia. Retrieved June 4, 2026. |