CrashSavers Trauma/Tourniquet/Self-assessment
| Part of | CrashSavers Trauma |
|---|
The learning experience and associated self-assessment are embedded in a learning environment in which gamification is employed to engage learners to complete both conceptual and practical activities. Results and immediate feedback for these activities are provided. To ensure that learners are practicing appropriate skills, the software-based simulation provides didactics and video-based instruction for the different hemorrhage control techniques.
Clinical case scenarios are built into the simulator as “games” and provide feedback based on the appropriate hemorrhage control technique selected. Advancement through the clinical case scenario is dependent on the learner’s responses.
| Incomplete answer | Incomplete steps to demonstrate understanding and adequate performance | Correct answer | Does not meet goal parameters | Completion of VR App & Simulator |
|---|---|---|---|---|
| Learner fails the scenario | Learner receives corresponding feedback | Learner moves onto physical simulator model | Learner receives specific feedback | Consider skill competency |
| Learner receives specific feedback on why other hemorrhage control techniques are more appropriate | Learner receives real-time feedback (i.e. visual cessation of hemorrhage with adequate technique) |
Case 1
[edit | edit source]Identifying Data: 32-year-old man
History: The patient is the driver of a light vehicle involved in a head-on collision traveling at 120 km/hr. The passenger of the vehicle has died.
Vital Signs:
- HR 142 bpm
- BP 70/30
- RR 34
- GCS 10 (M5, V2, E3)
- Shock Index 2.02
Physical Exam:
- Head: Laceration to the left parietal-temporal scalp with copious active bleeding. Bilateral palpebral edema and hematoma with anisocoric, hyporeactive pupils.
- Neck: No signs of trauma.
- Torso: Excoriated lesion in the left hemithorax from 2nd-7th costal arches. Crepitus is present upon palpation. Decreased respiratory sounds in the left hemithorax. Abdomen non-tender. Hematoma present in the let lumbosacral region.
- Extremities: Left upper extremity with expanding hematoma and deformity. Supracondylar traumatic amputation of the left lower extremity without active bleeding.
Analysis:

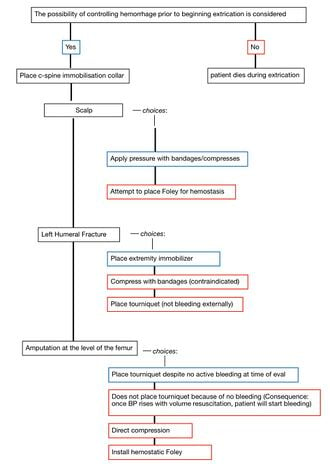
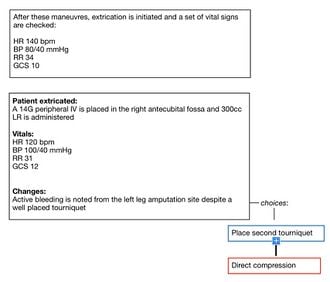
Case 2
[edit | edit source]Identifying Data: 21-year-old man
History: Firearm injury to the right inguinal region
Vital Signs:
- HR 115 bpm
- BP 100/70
- RR 26
- GCS 13 (M5, V4, E4)
- Shock Index 1.15
Focused Physical Exam:
- Head/Neck/Thorax/Abdomen/Pelvis: No signs of trauma.
- Extremities: Single 1cm diameter hole in the inner third of the right inguinal region with pulsatile active bleeding. Distal right extremity is cool with diminished pulses and capillary refill greater than 3 seconds. No motor or sensory defects.
Analysis:
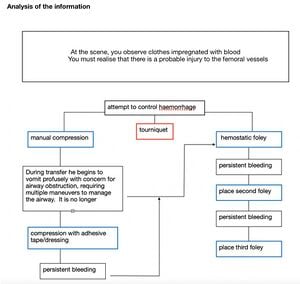
Case 3
[edit | edit source]Identifying Data: 38-year-old woman
History: Victim of domestic violence who presents with multiple blunt traumatic injuries and a stab injury from a broken bottle to the left axillary region.
Vital Signs:
- HR 135 bpm
- BP 130/90
- RR 32
- GCS 15
- Shock Index 1.03
Focused Physical Exam:
- Head: Palpebral hematoma on the left, swelling and deformity of the nasal pyramid, no active bleeding.
- Neck: No evidence of injury.
- Thorax: Right scapular hematoma. Normal chest expansion, no crepitus or subcutaneous emphysema.
- Abdomen/Pelvis: No signs of trauma.
- Extremities: Irregular wound with loss of soft tissues in the left axillary region, approximately 11cm in diameter with non-pulsatile active bleeding. Distal pulses are symmetric, capillary refill <3 seconds, and no motor or sensory defects.
Analysis:
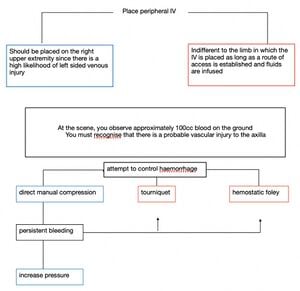
Case 4
[edit | edit source]Identifying Data: 21-year-old man
History: Patient found on a public street after multiple firearm injuries.
Vital Signs:
- HR 123 bpm
- BP 96/53
- RR 28
- GCS 15
- Shock Index 1.28
Physical Exam:
- Head: No injuries.
- Neck: 0.5cm orifice in zone 2 of the left neck with active pulsatile bleeding.
- Thorax: Symmetric ventilation. 0.5cm hole in the right infraclavicular region in the middle third of the clavicle, with an expanding hematoma.
- Abdomen/Pelvis: No injuries.
- Extremities: Left forearm with excoriation and projectile burn lesion measuring 10x2cm with minimal active bleeding. Distal pulses palpable and symmetric, capillary refill <3 seconds, intact distal motor and sensory function.
Analysis:

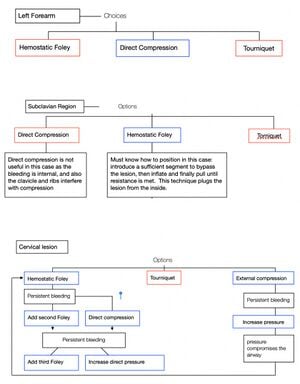
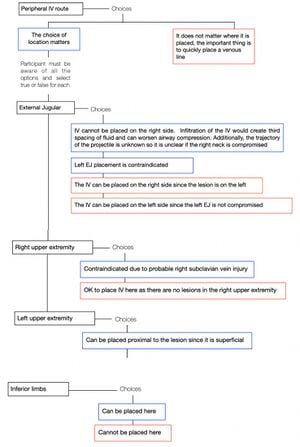
Skills Measurement
[edit | edit source]The self-assessment is based on clinical case scenarios in the VR app. Skills acquisition is assessed via training on the physical simulator constructed by the learners. Once all exercises have been completed, learners will be able to evaluate themselves and measure the time to placement of the tourniquet using a checklist adapted from Weiman (2019).[1]


As part of the assessment, we also created a platform to track learners’ performance data for completed clinical case scenarios.
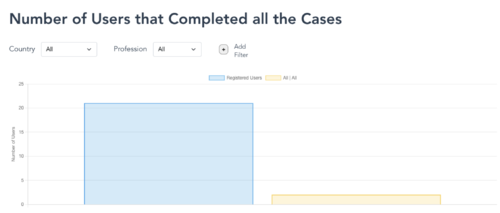
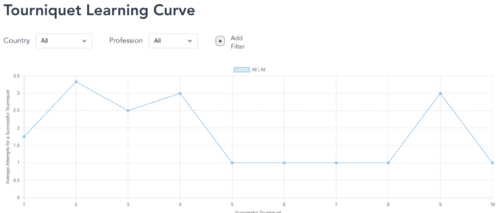
References
[edit | edit source]- ↑ Weinman, S. (2020). Retention of tourniquet application skills following participation in a bleeding control course. Journal of Emergency Nursing, 46(2), 154-162.
| Authors | CrashSavers |
|---|---|
| License | CC-BY-SA-4.0 |
| Organizations | Global Surgical Training Challenge |
| Cite as | CrashSavers (2021–2026). "CrashSavers Trauma/Tourniquet/Self-assessment". Appropedia. Retrieved June 4, 2026. |