PTC Course/Head Trauma
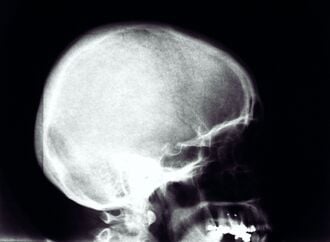
Head trauma is a major cause of death and disability in children and adults. Rapid and effective assessment and management in the Primary Survey saves lives and reduces disability. Hypoxia[1] and hypotension[2] significantly increase mortality[3] of head-injured patients. The most important management priorities in a head injured patient are opening the airway, giving oxygen and maintaining a good blood pressure.
Any patient with a head injury must have the cervical spine protected and immobilised.
Primary Brain Injury
[edit | edit source]Is the damage that occurs at the moment of trauma when tissues and blood vessels are stretched, compressed or torn.
Secondary Brain Injury
[edit | edit source]Results from brain swelling, hypoxia and high intracranial pressure - occurs after initial insult.
Early assessment and management of the Airway, Breathing and Circulation in the Primary Survey can prevent it.
- Primary Survey
- Airway and Cervical Spine
- Breathing
- Circulation
- Disability
- Pupil Size
- AVPU/GCS
- Secondary Survey
- Full Neurological Examination
Good clinical assessment can lead to early recognition of some important brain injuries that can be managed immediately or referred for surgery early. It is important to treat what you can within your expertise and resources.
The Glasgow Coma Score (GCS) reflects level of consciousness, and should be done repeatedly and complemented by neurological examination to look for signs of focal brain abnormality such as unequal pupils or limb weakness.
Hypotension or a recent epileptic seizure can make GCS interpretation difficult. Decline in the GCS or developing focal deficits can mean that there is an intracranial problem which needs treatment.
| Eye Opening (4) | Spontaneously | 4 | GCS 8 or Less: Severe Head Injury
GCS 9-12: Moderate Head Injury GCS 13-15: Minor Head Injury |
|---|---|---|---|
| To Voice | 3 | ||
| To Pain | 2 | ||
| None | 1 | ||
| Verbal (5) | Normal | 5 | |
| Confused Speech | 4 | ||
| Inappropriate Words | 3 | ||
| Inappropriate Sounds | 2 | ||
| None | 1 | ||
| Best Motor Response (6) | Obeys Commands | 6 | |
| Localises Pain | 5 | ||
| Flexes Limbs Normally to Pain | 4 | ||
| Flexes Limbs Abnormally to Pain | 3 | ||
| Extends Limbs to Pain | 2 | ||
| None | 1 |
If CT Scanning is available, this should be done, guided by the criteria in the table below
| Criteria for CT Scan in Head Injury (If Available) | |
|---|---|
| GCS <13 on initial assessment | In addition, adult patients who have experienced some loss of consciousness and amnesia since the injury and:
|
| GCS <15 at 2 hours after injury | |
| Suspected open or depressed skull fracture | |
Any sign of basal skull fracture
| |
| Post-traumatic seizure | |
| Focal neurological deficit | |
| More than one episode of vomiting | |
| Amnesia for events > 30 min before impact | |
Concerning Signs and Symptoms
[edit | edit source]Watch out for:
- Drowsiness or excessive sleepiness
- Confusion or disorientation
- Severe headache, vomiting or fever.
- Limb weakness
- Inequality of pupils
- Convulsions, seizure or unconsciousness
- Discharge of blood or fluid from ear or nose
Repeat Assessment
[edit | edit source]Remember:
- Deterioration may occur due to further bleeding in or around the brain.
- Regular review with repeated GCS and neurological observations are important
- Unequal or dilated pupils may indicate an increase in intracranial pressure
- Head or brain injury is never the cause of hypotension in the adult trauma patient - look for another cause.
The Cushing[11] Reflex
[edit | edit source]The Cushing reflex is a specific response to a severe rise in intracranial pressure, and is a late and poor prognostic sign.
The signs are:
- Low Heart Rate (Bradycardia)
- Widened Pulse Pressure
- High Systolic Blood Pressure (Hypertension)
- Low Diastolic Blood Pressure
- Irregular Respiration
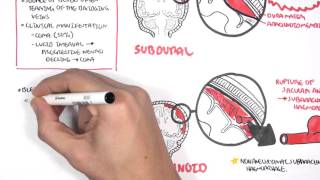
Traumatic Intracranial Pathology
[edit | edit source]The following conditions are potentially life-threatening but difficult to treat in district hospitals.
Extradural haematoma commonly results after an impact to the head. It results from bleeding from an artery often associated with a skull fracture. Often there is little primary brain injury and so rapid treatment may offer a good outcome.
Features of acute extradural haematoma include:
- An initial loss of consciousness after the impact
- The patient may wake up (lucid interval)
- Then rapid deterioration and unconsciousness
- Arterial bleeding with rapid increase in intracranial pressure
- Boggy scalp swelling over the site of the fracture
- The development of paralysis on the opposite side with a fixed pupil on the same side as the impact to the head.
Acute subdural haematoma commonly occurs in association with severe head injury. It results from bleeding from blood vessels around the brain and may be associated with significant primary brain injury.
Features include:
- Venous bleeding and clotted blood in the subdural space
- Frequently, severe bruising or damage to the underlying brain
Management
[edit | edit source]After the Primary Survey, the management of these injuries is surgical. If possible make a rapid transfer to a hospital where neurosurgery can be done. If this is not possible and if appropriate skills are locally available, an exploratory burr-hole[16] should be made immediately for diagnosis/drainage on the side of the dilating pupil.
Additional Pathology
[edit | edit source]The following conditions may sometimes be treated with more conservative medical management (Airway, Breathing, Circulation and regular monitoring and observations), as neurosurgical intervention is often not indicated initially.
Signs include:
- Bruising of Eyelids - Racoon Eyes[18]
- Bruising over Mastoid Process - Battle’s Sign[19]
- Cerebrospinal Fluid (CSF) Leak from Ears[20] And/Or Nose[21]
Cerebral Concussion[22]
[edit | edit source]With temporary altered consciousness.
Closed Depressed Skull Fracture[23]
[edit | edit source]Without neurological deficits.
Intracerebral Haematoma
[edit | edit source]May result from acute injury or progressive damage secondary to brain bruising (some haematomas may expand by late bleeding/oedema to cause mass effect and delayed clinical deterioration).
With altered conscious level but no haematoma on CT scan.
Management
[edit | edit source]The priority of management is stabilisation of the airway, breathing and circulation, with immobilisation of the cervical spine.
Keeping the oxygen level as high as possible and the systolic blood pressure above 90mmHg is the most important aim in emergency treatment for patients with head injury.
Specific further management consists of:
- Stabilisation of ABC.
- Immobilise the cervical spine.
- Continuous oxygen.
- Supporting and controlling ventilation; avoid CO2 rise.
- Intubation if severe head injury with CGS <8.
- Monitoring of vital signs, pupils and regular neurological observations (including repeated GCS measurement).
- Elevate the head of the bed if possible, without bending the neck.
- Keep the temperature stable.
- Do not withhold pain relief, but take care not to make the patient too drowsy.
- Mannitol 20% infusion may reduce intracranial pressure. Its best use is to allow short-term benefit before obtaining a CT scan or transfer to a neurosurgical facility
- If CT scan is not immediately available and an intracranial haematoma suspected due to clinical deterioration, exploratory burr holes may be indicated.
Note
[edit | edit source]Alteration of consciousness is the hallmark of brain injury.
References
[edit | edit source]- ↑ https://my.clevelandclinic.org/health/diseases/23063-hypoxia
- ↑ https://my.clevelandclinic.org/health/diseases/21156-low-blood-pressure-hypotension
- ↑ https://www.ahajournals.org/doi/10.1161/circ.130.suppl_2.4
- ↑ https://stanfordhealthcare.org/medical-conditions/brain-and-nerves/acquired-brain-injury/types.html
- ↑ https://teachmesurgery.com/neurosurgery/traumatic-injuries/assessment-head-injury/
- ↑ https://www.youtube.com/watch?v=0hhcxaeOCYs&ab_channel=GeekyMedics
- ↑ https://www.youtube.com/watch?v=-7ERNH_o5Ss&ab_channel=GeekyMedics
- ↑ https://www.youtube.com/watch?v=sJBpai74tlU&ab_channel=GeekyMedics
- ↑ https://geekymedics.com/glasgow-coma-scale-gcs/
- ↑ https://radiopaedia.org/articles/computed-tomography?lang=gb
- ↑ https://www.osmosis.org/answers/cushings-triad
- ↑ https://radiologyassistant.nl/neuroradiology/hemorrhage/traumatic-intracranial-haemorrhage
- ↑ https://www.youtube.com/watch?v=Kb_wzb7-rvE&ab_channel=ArmandoHasudungan
- ↑ https://teachmesurgery.com/neurosurgery/traumatic-injuries/extradural-haematoma/
- ↑ https://teachmesurgery.com/neurosurgery/traumatic-injuries/subdural-haematoma/
- ↑ https://www.youtube.com/watch?v=QeDQZoeg0RA&ab_channel=EM%3ARAPProductions
- ↑ https://radiopaedia.org/articles/basilar-fractures-of-the-skull?lang=gb
- ↑ https://radiopaedia.org/articles/raccoon-eyes-sign-base-of-skull-fracture?lang=gb
- ↑ https://radiopaedia.org/articles/battle-sign-base-of-skull-fracture?lang=gb
- ↑ https://radiopaedia.org/articles/csf-otorrhoea?lang=gb
- ↑ https://radiopaedia.org/articles/csf-rhinorrhoea?lang=gb
- ↑ https://www.aans.org/en/Patients/Neurosurgical-Conditions-and-Treatments/Concussion
- ↑ https://radiopaedia.org/articles/depressed-skull-fracture?lang=gb
- ↑ https://teachmesurgery.com/neurosurgery/traumatic-injuries/diffuse-axonal-injury/
| Authors | Matthew Arnaouti |
|---|---|
| License | CC-BY-SA-4.0 |
| Cite as | Matthew Arnaouti (2022–2025). "PTC Course/Head Trauma". Appropedia. Retrieved June 4, 2026. |