Training in Primary Assessment is included in this California-based EMT program as it is required in each of the higher level scenario-based skills tested for California Registration.[1]
The purpose of the Primary Assessment/Survey is to identify and treat life threatening conditions. The Primary Assessment/Survey should be performed rapidly and methodically. If massive hemorrhage is present it must be controlled first. Manage or direct the management of potentially life threatening issues as they are encountered.
The following is a Primary Assessment/Survey of a conscious patient which primarily follows the X-ABCDE mnemonic (with an X for eXsanguinating hemorrhage). If the patient is Unresponsive follow the Circulation, Airway, Breathing (CAB) assessment per American Heart Association (AHA).
Scene Size Up:
The only assessment that is done prior to the Primary Assessment/Survey is the Scene Size-Up which can be accomplished using the PENMAN mnemonic.
General Impression[edit | edit source]
Determine the following as you approach the patient: Does the patient appear Conscious or Unconscious? Does the patient appear to be breathing? if so is the breathing Labored or Unlabored. Are there any obvious abnormal skin colors and are there any body fluids near the patient? Using these three assessments determine if the general impression is poor or good.
Note: By definition a poor general impression indicates a priority patient
Responsiveness/Level of Consciousness[edit | edit source]
Determine LOC using the AVPU scale and categorizes the patient as Alert, Verbal, Painful or Unresponsive. If significantly impaired, use the Glasgow Coma Scale to grade.
Chief Complaint/Apparent Life Threats[edit | edit source]
Identify yourself, attempt to reassure the patient, obtain consent, determine the patients name and the chief complaint. If the patient is conscious, this may be performed at the same time as XABCDE assessment. For example:
Hi my name is___________________________. I am an EMT, I'm going to help you out as best I can, is that OK? What is your name? What is affecting/hurting you the most right now?? (Did you hurt your head, neck or back? Did you fall down? Is it possible you lost consciousness)
Note: If exsanguinating hemorrhage if present must be controlled immediately even prior to assessing the Airway. Until proven otherwise an apparent life threat can be the chief complaint i.e. chest pain or shortness of breath.
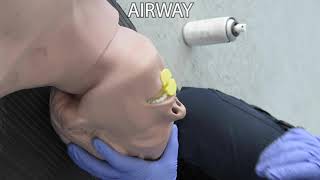
X-Airway[edit | edit source]
X: Exsanguinating Hemorrhage if present must be controlled prior to assessing the Airway. Severe extremity bleeding should be controlled with Direct pressure and/or application of a tourniquet. Severe external hemorrhage from wounds to the trunk or junctions should be controlled by direct pressure, packing (preferably with hemostatic gauze), junctional tourniquets and/or pelvic binder.
Assess Airway: Count the number of words the patient uses in a sentence, assess the ease of speaking, and listen for air exchange and any abnormal sounds, note chest rise.
Snoring = Obstruction by tongue (position airway and insert adjunct)
Gurgling= fluids in airway, blood, vomitus etc. (suction immediately, manually clearing)
Stridor =upper airway obstruction (Anaphylaxis?, Edema?)
Wheezing=lower airway obstruction (Asthma?)
Manage Airway: If for any reason the patient is not able to manage their own airway implement the appropriate intervention. Position-Head-tilt chin lift or Trauma Jaw thrust as needed, manual clearing-turn patient and wipe out large amounts of fluids, Suction-secretions,blood, vomitus etc., Place an airway adjunct (OPA/NPA), BLS obstructed airway maneuvers if appropriate.
Note: No airway, no patient! A noisy airway is an obstructed airway! A patent airway is imperative to the survival of the patient. It is the EMT's responsibility to obtain and maintain a patent airway throughout patient contact, through timely and appropriate interventions and frequent reassessment as necessary.
Breathing[edit | edit source]
Assess: Determine the rate and depth of respirations. (A rate < 8 or > 24 breaths/min necessitates prompt treatment.[2]) Look for accessory muscle use. Note positions that might indicate respiratory distress (tripod, bolt upright, splinting). Prior to performing a hoop test ask, "Do you have anything sharp on you that might poke or cut me?" Advise patient that you are going to place your hands on the sides of their chest and ask them to take a deep breath. Note if they experience increased pain upon deep inspiration. Feel for equal chest rise. Do a quick listen-auscultate lungs sounds in the midaxillary region once on each side. (A more thorough auscultation will occur during the vital signs assessment.) Note presence of cyanosis or other abnormal skin signs.
Manage: If necessary intervene with positioning, BVM, Oxygen, coaching, recognizing a flail segment/pneumothorax, sealing sucking chest wounds.
Note: It is imperative that if a patient has respiratory distress that the rescuer, auscultate lung sounds(quick listen), palpate the chest wall and visualize the chest.
Circulation[edit | edit source]
Assess: Palpate appropriate pulse point (radial on the conscious patient, carotid on the unconscious patient[3]). Is the pulse present or absent? If radial pulse is absent assess carotid or femoral pulse, determine quickly if the pulse rapid vs slow, strong/bounding vs weak & thready, regular vs irregular, check capillary refill, assess skin signs (Color, Temperature, Moisture), Clear the kill zone (Question or palpate as appropriate) and control any significant bleeding found. In the unconscious patient, this is the first step in the primary assessment.
Manage: Position patient appropriately, control bleeding, provide warmth as necessary. If the patient was unconscious and there is no palpable carotid pulse, begin CPR.
Note: Capillary refill while most useful on children under the age of six in a normothermic environment can still be useful on adults when taken in clinical context with other data points.[4]
Disability[edit | edit source]
Assess: Alterations in level of consciousness. the simplistic AVPU scale has already been assessed, now score the patient using the Glasgow Coma Scale (GCS) to establish a baseline of cerebral function, which can then be used to compared to serial GCS assessments. The GCS is the most common, reliable, and consistent method of neurological and mental status assessment. When using the GCS the most important assessment is the motor assessment which has been shown to independently be as effective as the total GCS score in the prediction of 5 trauma outcomes: emergency intubation, clinically significant brain injury, need for neurosurgical intervention, Injury Severity Score greater than 15, and mortality.[5] If the patient has an altered level of consciousness quickly assess pupils.
Manage: Care for the altered level of consciousness includes remaining aware of the need to protect the airway. Specific interventions will depend upon the cause of the altered mentation.
Note: A patient who has an altered level of consciousness and is uncooperative or antagonistic may be suffering from poor cerebral perfusion, TBI, Drug/ETOH/toxic exposure or metabolic derangement.
Exposure[edit | edit source]
Expose/Examine: Critical Trauma Patient-Remove clothing for assessment. Non-Critical Trauma patient-remove only the clothing necessary to perform the assessment.
Environment: Once assessment/interventions are complete immediately take steps to protect patient from the environment and to protect modesty. Keep the trauma patient warm!
Patient Priority/Transport Decision[edit | edit source]
- State patient Priority
- Describe how & when to move the patient to gurney and to ambulance
- State steps to be taken on scene prior to movement
- State destination
Note: Once the primary survey has been completed the rescuer can now definitively state patient priority. The knowledge gained from the scene size up, primary survey and situational awareness of hospital locations and transport times allows the rescuer to describe how & when to move the patient and state steps to be taken on scene prior to movement to gurney or ambulance. The rescuer can also state destination at this time based on the needs of the patient. (Trauma center, Stroke center, STEMI receiving facility, burn center, patient desire, etc.). Local protocols, medical direction, and time to definitive care will dictate if an EMT calls for an ALS backup to provide transport or initiate transport directly.
Documentation[edit | edit source]
Documentation of the Primary Assessment should be included in the Patient Care Report (PCR) in the form:
- Example for stable patient: "Patient sitting upright in kitchen chair, patient tracks EMS upon approach. Patient skin signs normal colored and dry, patient exhibits no respiratory distress. Patient answers all questions appropriately in full word sentences and follows directions. Initial patient assessment reveals no obvious life threats or bleeding. Secondary assessment unremarkable. Patient AxO 4, GCS 15, GFAST negative, pupils 4 mm PERRL. Patient ambulated to gurney without ataxic gait or abnormal weakness."
- Example for patient with neurological deficit following fall: "Patient found sitting slumped against the wall in bathroom, patient tracks EMS upon approach. Patient skin signs normal colored and dry, patient exhibits no respiratory distress. Patient answers all questions appropriately in full word sentences with significant slurring present. Patient follows directions with unilateral weakness to the right upper and lower extremities and right sided facial droop. Patient assessment reveals oozing laceration to right temporal area, bleeding controlled by EMS with gauze bandage. Patient AxO 4, GCS 15, GFAST 3 with positive arm drift, facial droop, and slurred speech, pupils unequal at 3 mm (L) and 5 mm (R)."
- Example for completely unresponsive patient: "Patient found lying prone on ground with several empty bottles of alcohol in her immediate vicinity and vomit around her head. Patient does not track EMS upon approach, patient unresponsive to painful/noxious stimuli. ALS response requested. Patient has strong carotid pulse, patient airway suctioned to remove vomit. Patient is profoundly bradypneic. OPA placed without issue, patient ventilated via BVM at 12 breaths/minute. Patient displays peri-oral cyanosis, skin signs cold. Patient pupils pinpoint and minimally responsive. Secondary assessment reveals track marks on patient's left arm at the AC space. Patient GCS 3."
Self Assessment[edit | edit source]
- Practice the Primary Survey Skill Sheet until you are comfortable with the workflow
- Use the NREMT Trauma "Skill Checklist"
- For additional practice, have a fellow student test you with a Practice Trauma Scenario
- Test your knowledge with this quiz
Tips and Tricks[edit | edit source]
- In unconscious, unresponsive patients, the algorithm places more priority on circulation (CABDE) to ensure that CPR is not needed.
- If a patient presents with unequal pupils, ask if that is normal for them. Anisocoria, or slight pupillary size difference affects up to 20% of the population and is often benign. If the patient responds that they do not know if they normally have differently sized pupils, err on the side of best patient care and treat as though this is a new onset.
- For any assessment finding that is not what you would expect (i.e. normal for the majority of the population), ask if this is a normal finding for your patient. Many patients with a stroke history may have chronic deficits that can act as distractors to the true issue at hand.
- Set yourself up for success; if you know you have a trauma patient, preemptively starting the heat in the back of the ambulance allows time for the patient compartment to heat up and eliminates the need for you to remember to do so on scene.
Additional Resources[edit | edit source]
TBD - extra videos to watch, links to other pages for more reading
References[edit | edit source]
PHTLS: Prehospital Trauma Life Support 9th Edition by National Association of Emergency Medical Technicians (NAEMT)
- ↑ https://emsa.ca.gov/wp-content/uploads/sites/71/2017/07/Skills-Form-7.1.17.pdf
- ↑ Pollak, Andrew N. (ed.) (2021). Emergency Care and Transportation of the Sick and Injured (12th ed.). p. 356. ISBN 9781284246223
- ↑ Pollak, Andrew N. (ed.) (2018). Nancy Caroline’s Emergency Care in the Streets (8th ed.). p. 513. ISBN 9781284104882.
- ↑ McGuire, D. et al. (2021). Capillary Refill Time. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK557753/
- ↑ Hopkins, Emily et al. (2018). A Two-Center Validation of "Patient Does Not Follow Commands" and Three Other Simplified Measures to Replace the Glasgow Coma Scale for Field Trauma Triage. Annals of emergency medicine, 72(3), 259–269. https://doi.org/10.1016/j.annemergmed.2018.03.038