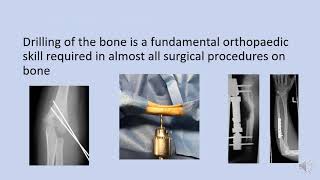
ETALO Bone Drilling Module
ETALO in the Ugandan language of Luganda means "bone infection". For us, ETALO is also an acronym that stands for Education To Advance Limb-Saving Options for Open Fractures and Osteomyelitis.
The ETALO team came together in 2020 for the Global Surgical Training Challenge (GSTC), building on previous extensive work by members of the team, to develop a low-cost simulator and training course for non-orthopedic clinicians to learn to drill bone as a central part of treatment of open fractures and osteomyelitis.
Syllabus
[edit | edit source]Phase 1: Knowledge Review
[edit | edit source]- The ETALO Approach to Self-Directed Learning and Self-Assessment
- Pre-Training Assessment
- Basics of Bone Anatomy and Drilling
- Osteomyelitis
- Open fractures
Phase 2: Simulator Build
[edit | edit source]- Overview of Building a Bone Simulator
- Building a Basic Bone Drilling Simulator
- The Plunge Detector
- Building a Simple Bone Simulator
- Building an Advanced Simulator
- Simulator Layer Options
Phase 3: Skills Practice
[edit | edit source]- Drilling Bone
- Removing a Cortical Window
- Placing a Half Pin
- Applying an External Fixator (coming soon)
Evaluation and Next Steps
[edit | edit source]Why we developed this training
[edit | edit source]Osteomyelitis and open fractures are common orthopaedic conditions throughout the globe, with particularly high prevalence in LMICs. Fractures from vehicular trauma are considered at epidemic proportions. Lack of access to early treatment leads to a high burden of unnecessary disability and death. The countries with the highest rates have the least skilled surgeons available. The skills of drilling bone to decompress and debride osteomyelitis, including sequestrectomy and saucerization, the debridement and external fixation of open long bone fractures, and the performance of a fasciotomy are skills that can be task-shifted to other clinicians in rural and district hospitals where there are not orthopaedic specialists. These skills are included amongst the 44 essential surgical skills listed by the World Bank Disease Control Priorities1. The goal of the ETALO bone drilling modules is to teach these fundamental surgical skills to providers in resource-limited settings.
The goal of the ETALO bone drilling module is to train medical students/officers, clinical officers and non-orthopaedic surgeons to become confident and competent in performing bone drilling in order to debride osteomyelitis and stabilize open fractures in resource-limited settings. Osteomyelitis and open fractures are very common in low and middle income countries (LMICs). These conditions require early intervention to debride and stabilize bone to avoid complications that would result in poor limb function, need for multiple surgeries, long-term disability, and possibly amputation. The surgical skill sets required to treat both conditions are related, both centering around the psychomotor skill of drilling bone - whether that be to drain pus from the intramedullary canal for infection management or to place pins for an external fixator to stabilize a bone to allow for healing in the setting of fracture or infection. This skill set is part of routine orthopaedic training, but not taught in non-orthopaedic surgical and medical programs. This is a problem because many places lack orthopaedic surgeons available in a timely manner, if at all, to render appropriate care. The task then falls to general surgeons, medical officers or clinical officers - none of whom receive formal training in drilling techniques and musculoskeletal surgical care.
Lack of Orthopaedic Surgeons: There are approximately 70 orthopaedic surgeons in Uganda, a country of over 43 million people. With few orthopaedic surgeons and over 80% of the population living in rural settings, infectious and traumatic injuries are frequently managed in district or regional hospitals. While these settings have general practitioners or general surgeons, such providers do not have orthopaedic training and are therefore not familiar with the basic skills necessary to treat these conditions. Consequently, patients may get sub-optimal care by inexperienced clinicians or may have significant delays in care due to the need for referral to a higher-level facility with orthopaedic specialists. Going to a major hospital frequently involves the family having to raise funds, so they care delay can be days to weeks.
The ETALO Project's bone drilling simulator and this training course were designed to contribute to improvement in outcomes for treatment of open fracture and osteomyelitis. There will be a decrease in morbidity, time to definitive care, and overall cost of care with a better trained clinical workforce.
The ETALO team has its roots in Uganda, but we hope the simulator and this training module will eventually be accessible for use throughout the world, particularly for those with limited resources.
Who is Team ETALO?
[edit | edit source]Our team is composed of orthopaedic surgeons, engineers, a public health education/assessment specialist, and a program manager/research coordinator. Here were the members and affiliations of Team ETALO during the GSTC Discovery Award Phase:
| Moses Muhumuza Fisha, MBChB, MMed (Ortho) - ETALO Lead | Orthopaedic Surgeon | CoRSU Rehabilitation Hospital | Uganda |
| Coleen S. Sabatini, MD, MPH - ETALO Co-Lead | Orthopaedic Surgeon | University California San Francisco | USA, Uganda |
| Norgrove Penny, CM, MD, FRCS(C), FCS(ECSA) | Orthopaedic Surgeon | University of British Columbia | Canada, Uganda |
| Qusai Hammouri, MD, MBBS | Orthopaedic Surgeon | Northwell Hospital | USA |
| Isaac Oluk (Discovery Award Phase) | Engineer | Badaye Technologies | Uganda |
| Julius Mugaga (Discovery Award Phase) | Engineer | Badaye Technologies | Uganda |
| Tayla Colton, ScM | Education and Assessment Lead | Independent Consultant | USA |
| Daniella Akellot, MPH | Project Manager/ Research Coordinator | CoRSU Rehabilitation Hospital | Uganda |
Overview of "Drill Down – A Guide to Drilling Bone"
[edit | edit source]Who is the ETALO "Drill Down" Training For?
[edit | edit source]The ETALO Drill Down Training Course was developed to aid in the training of medical students from all areas, medical officers stationed in rural parts of the world with no access to advanced training, and non-orthopedic practitioners who are faced with the need to care for patients with musculoskeletal problems requiring drilling of bone as a component of appropriate treatment like acute and chronic osteomyelitis or open fractures.
Our Focus on Self-Directed Training and Self-Assessment
[edit | edit source]The ETALO "Drill Down" training is self-directed so that learners can remain in their place of work or home instead of traveling for often costly and time-intensive in-person training. Learners can go through these modules at their own pace. Although a learner can complete all aspects of the online curriculum and self-built in-person simulator on their own, leaners are encouraged to work with one or more learning partners as they move through the training, build their simulator, and develop their bone drilling skills. Learners can build their own simulator models with locally sourced materials. They will follow a set of instructional modules which rely on short, practical educational videos (which can be watched as many times as needed) to help them in building the simulator and using it to learn the psychomotor skill of drilling bone. Several methods of self-assessment are integrated into the ETALO "Drill Down" training module so that learners can frequently and deliberately assess their knowledge and psychomotor skills and use self-assessment information as a tool for continued improvement.
Overview of the ETALO Bone Drilling Simulator Model
[edit | edit source]The ETALO simulators allow for learners to build the psychomotor skills required for drilling bone and placing pins (for external fixation and traction). The simulators can be made by the learners from locally-available items. After building a simulator and reviewing the ETALO instructional videos on bone drilling, the user can practice drilling bone.
When drilling bone in a live patient, control of the drill is imperative. Should the operator slide off the bone or drill too far beyond the far cortex of the bone, important anatomic structures can be injured. If a nerve is injured, the patient could have numbness/paralysis or both. Should an artery be injured, the patient could lose blood flow to the foot or hand. Slipping off the slides is obvious to the user, but plunging too far cannot be seen by the user while they are drilling. As such, we developed a "plunge detector" that will either trigger a lightbulb or a buzzer if the user has drilled too far past the far cortex.
We have developed three different physical simulators of increasing complexity, with a matrix of options for each:
- Basic simulator which is just a hollow tube to simulate bone
- Simple simulator which includes simulation of bone and periosteum and includes a "plunge detector" to alert the learner if they have drilled too far past the far cortex.
- Advanced simulator which is the simple simulator with the addition of muscle and skin to simulate normal human anatomy.
The ETALO Drilling Curriculum includes a self assessment tool that allows the learner to gauge their improving skills with regard to drilling bone. Learners can either work alone or we have also incorporated an element of trainees working in teams to assess each other or a mentor and trainee assessment
Syllabus
[edit | edit source]This simulator and curriculum were developed to aid in the training of a range of learners - medical students from all aspects of the medical world, medical officers stationed in rural parts of the world with no access to advanced training, clinical officers, and non-orthopedic surgeons who are faced with the need to provide urgent care to a patient to save a limb, such as in cases of acute and chronic osteomyelitis or open fractures.
The bone drilling simulator module is presented in a three-part format that includes:
- Building the simulator
- Practicing with the simulator with the aid of teaching videos
- Self and/or group assessment
See #Syllabus for the complete, up-to-date syllabus.
Getting Started
[edit | edit source]This video will provide you with basic information about why being able to drill bone is important for the care of patients and why the work of ETALO is important globally.
Innovation
[edit | edit source]The most common simulator used for external fixation is the synthetic composite bone (Sawbones) which can be expensive to purchase and ship and are therefore not available to those practicing in LMICs.
Our models are affordable and locally-sourced and we give the user an array of options for materials to use in their simulator. For example, a user could start their training using PVC pipes to practice the skill of drilling and not plunging , and then graduate to animal bones, of varying sizes to further develop their skills with a more "human-like" bone feel. Finally they can choose to perfect their skills once developed on 3D printed models of human bone. Additionally, in environments with access to basic computers, training will be further enhanced with the use of virtual CAD models. Our plan is to release the virtual CADmodel to an open source platform with clear documentation to allow a wider community of users and developers to engage with the technology wherever they are located hence encouraging improvements.
By providing an array of options to train on, our models allow the user to choose the more affordable options initially, and then the more realistic options as they gain skills.
Evaluation
[edit | edit source]The original bamboo and PVC pipe bone simulator prototypes including the self assessment forms were tested among Orthopaedic Surgeons, Medical and Orthopaedic officers during a training in Mbale district, Eastern Uganda. These participants were requested to drill the prototypes and assess themselves using the self assessment forms. Feedback from this evaluation was provided to the ETALO team so as to make adjustments to the prototypes and the self assessment forms.
-
ETALO Team Lead shows an orthopaedic surgeon how to use the self assessment form.
-
An orthopaedic surgeon drills the bone simulator prototype.
-
A medical officer drills the bone simulator prototype
-
An orthopaedic officer fills the self assessment form after drilling the bone simulator prototype.
The original animal bone simulator prototype and self assessment forms was tested among lay people living in New York. Participants were requested to drill the animal bone prototype and to assess themselves using the self assessment form. The feedback obtained from this session was given to team ETALO members so as to make adjustments to the prototype and self assessment forms.
Modifications based on the feedback obtained from this evaluation have been made to the original prototypes to produce improved bone simulators.
Adoption
[edit | edit source]Potential Users: Undergraduate students, medical officers/general practitioners, (orthopaedic) clinical officers, general surgeons, orthopedic surgery residents and orthopedic surgeons.
The Need: Drilling human bone is a skill that is necessary for all aspects of orthopaedics, including management of fractures and infection and even placement of intraosseous lines in emergency situations. Drilling techniques are most commonly taught in orthopaedic residency programs. Thus, those medical providers who don't do orthopaedic residency programs often do not learn this skill. Therefore when general surgeons and medical officers/general practitioners are confronted with patients at the district/rural hospital level, they are not comfortable rendering the necessary immediate care because they have not practiced the fundamental skill needed to stabilize or decompress a bone. Thus, the main users for this model will be medical students preparing for their medical officer service, medical officers who are currently working in the community, and general surgeons in areas where orthopaedic surgeons are not readily available. Additionally, this model can be adopted by orthopaedic surgery training programs in LMICs for training their junior residents on drilling techniques and external fixator placement to enhance their skills as they are also learning to operate on real patients.
The clinical utility of this model will likely be obvious to the target audience, but making it acceptable and accessible both in terms of materials and cost will be most crucial. Accompanying the model must be clear educational information on when and how to perform the skill and when and how to recognize that a higher level of care is needed for a patient. Educating people about the availability of the module will be imperative for adoption and therefore, will need to market it effectively to the target users through educational and social media focused on medical students, trainees and surgeons.
In addition to our transcontinental group of clinical, research, academic and service delivery organizations, two of our technical experts are also affiliated with the private sector (Badaye Technologies Ltd- www.badayetechnologies.com) - with dedicated R&D, design, simulation and local technological manufacturing expertise in Uganda and thus will provide a crucial project partnership for both technical expertise and frugal manufacturing capabilities for easy adoption and access to the technology by the local community.
Reproducibility
[edit | edit source]To ensure reproducibility and affordable production, our simulators were developed and tested in Uganda. Fabrication of iterations of the simulator will be possible, and tested, in even very remote locales. Reproducibility is ensured by Uganda, being in the lowest tercile of development globally (159 out of 189), as proxy for any low income country.
To ensure reproducibility, we will include the following in our handover documentation:
- List of specific supplies needed to build the simulator
- A table of material options for the simulation highlighting what materials are ideal for beginning, intermediate and advanced skills, and what bones of the human they most closely resemble.
- Budget guide and template for replication of the simulator
- Step-by-Step Instructions on how to assemble the simulator
- Instructional video on how to assemble the simulator
- Self-assessment instructions and tools, including learning targets and rubrics with benchmarks
- Guidelines for infrastructure assessment of the user's local healthcare facility (To answer the question of "should this procedure be done at this healthcare facility?")
- List of surgical specific supplies needed to perform procedure in for simulation (To answers the question, "do you have the surgical equipment needed to do these procedures at your healthcare facility?")
We made the design choice to offer different material options for the end user as the cost of different material might vary based on geography/proximity to major cities, locally available materials, etc.. We hope this will allow the end user to choose the more affordable options that allow for the skill level they are attempting to acquire.
Accessibility
[edit | edit source]Simulation Material (Material user will drill) :
Our target user will be able to purchase two of the simulation material at the local market (pipes and animal bones) which are affordable and readily available. The 3D printed bone models are a more advanced and expensive option but will be able to be printed locally using the open source file we will provide. There are 3D printers in a variety of places in Uganda including at CoRSU Rehabilitation Hospital and government innovation centers.
Surgical Tools:
To be able to perform the simulation the user will have to have access to drills, half pins and external fixators. These may be borrowed from the local hospital or medical education facility. Hand drills can be purchased locally if not available from the hospital. If half pins are not available they can be substituted with long fully threaded construction screws
Simulation Set up:
The set up will be quite straightforward. What is required will be a flat stable surface (a table), the bone model, and a drill. We will incorporate a clamp or other holding device into the model to stabilize the model for drilling (or can be held by a colleague)
By providing an array of bone simulator options to train on, our model would allow the user to choose the most affordable option initially, and then the more challenging option as they gain skills, and then finally to add nuance into their skill set by practicing on bones that simulate different types of more challenging bone (e.g. osteoporotic, small diameter, etc).
The set up of the simulator will be straightforward and instructions will be laid out in both written and video form.
| Authors | ETALO |
|---|---|
| License | CC-BY-SA-4.0 |
| Organizations | Global Surgical Training Challenge |
| Cite as | ETALO (2021–2026). "ETALO Bone Drilling Module". Appropedia. Retrieved May 30, 2026. |