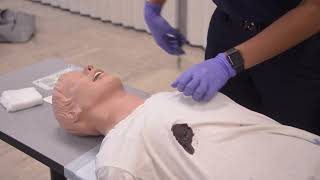
Treatment of Penetrating Chest injury is included in this California-based EMT program as it is required for skills verification for California Registration.[1]
Penetrating chest trauma most frequently involves mechanisms such as stabbing and gunshot wounds (GSW), although there are a variety of ways the chest can be penetrated in industrial accidents.
Penetrating chest trauma frequently creates serious or fatal injury because of injuries to the lungs and large vascular structures (including the heart) that are housed within the chest cavity. You should have a high index of suspicion that there may be C-spine involvement in any trauma involving the chest, and take appropriate precautions during treatment.[2] Prehospital treatment is limited to life support measures such as oxygen while stabilizing and sealing the chest cavity with rapid transport, but these can be critical to help the patient survive long enough to reach definitive care.
Patient Exam[edit | edit source]
In a patient with blunt or penetrating chest trauma, you may encounter a collapsed lung, called pneumothorax, or a significant amount of blood in the chest cavity, called a hemothorax. Be particularly alert for signs of a tension pneumothorax, in which the air pressure inside the chest cavity is increasing and pressing on vital structures. This is a medical emergency that can quickly lead to the death of the patient if left untreated.[3]
The prehospital management of chest trauma starts with a thorough examination for the following signs and symptoms:
- Unequal chest rise and fall, paradoxical motion, or chest deformity which can indicate underlying rib fractures
- Respiratory distress, including dyspnea, tachypnea and patient reported pain with breathing
- Abnormal or absent lung sounds which can indicate airway blockage or the presence of a pneumothorax
- Distended neck veins as well as tracheal deviation away from the affected side indicate a tension pneumothorax. Tracheal deviation is a late sign of tension pneumothorax.[4]
- Signs of shock including hypotension, and tachycardia may result from blood loss or impaired cardiac output secondary to a tension pneumothorax.[5]
- Altered mental status which can indicate that the patient is not oxygenating or perfusing properly
- Subcutaneous emphysema or Soft Tissue Crepitus, in which air has been pushed by the pressures of respiration into the subcutaneous tissue of the chest and neck. This air can be felt as a crackling sensation upon palpation of the skin and should be looked for as a sign of pneumothorax in the unresponsive patient.[6]
Be alert to the signs of tension pneumothorax, and have a high index of suspicion that one may develop in any situation with a chest wall injury.
Also ensure that you have examined the patient's entire chest when you suspect chest trauma, as entrance/exit pairs of wounds, and multiple injuries are commonly missed.
Treatment[edit | edit source]
The majority of chest wall injuries can be stabilized with supplemental oxygen, and the placement of an occlusive dressing with an integrated valve on the chest wound (known as a chest seal). Following examination, to stabilize and prepare a patient with a penetrating chest wound for transport:
- Open and Assess the airway. Maintain c-spine precautions as warranted.
- Apply direct pressure with a gloved hand to any penetrating wounds.
- Administer oxygen as needed. Use a non-rebreather mask, depending on the patient condition and needs. If needed, assisted ventilations with a BVM may be performed, however positive pressure ventilation should be used with caution as it can worsen a tension pneumothorax by pushing pressurized air into the thorax through a lung laceration.
- Stabilize the chest wall in the case of Flail Chest or other significant deformity.
- Apply Occlusive Dressings to all of the penetrating wounds. There are many types of commercial and improvised occlusive dressings available, but the most important characteristic is that air is prevented from entering the chest cavity in inhalation and allowed to exit upon exhalation:
- Special purpose commercial chest seals usually have an adhesive to secure to the chest wall and a ventilation valve that will allow air to escape and not re-enter. These may be too bulky to place on the patient's back if the patient is to be transported supine.
- Improvised chest seals may be created from many of the air-impermeable materials readily available to the EMT including Tegaderm, gloves, vaseline impregnated gauze, foil, etc. Most improvised seals will require medical tape to secure them. Many EMS systems recommend securing the improvised seal by taping 3 to 4 sides of the dressing leaving a corner or side untaped to allow air to escape. However, if air is re-entering the wound, it is preferable to tape the entire circumference.[7]
- Transport. Even with a successfully closed wound, the chest may still be bleeding freely, and undetectably into the pleural cavity. Rapid transport and early surgical intervention is the definitive management of penetrating chest injuries. Immediate transport and ALS back up is warranted.
Pathophysiology of Pneumothorax[edit | edit source]
A pneumothorax is any a condition in which air leaks into the chest cavity through a defect in the lung, the chest wall, or both, and collects in the pleural space. Understanding the pathophysiology of the pneumothorax can help you interpret the physical findings and understand the effects of certain interventions. The EMT should understand how positive pressure ventilation can worsen a pneumothorax or lead a simple open or closed pneumothorax to becoming a tension pneumothorax.
- An open pneumothorax, sometimes referred to as a "Sucking Chest Wound", involves the penetration of the integrity of the chest wall. Upon inspiration, the expansion of the chest cavity means the air pressure inside the thorax is below the atmospheric pressure, and air is "sucked" into the chest cavity through the wound. Upon expiration, the air may escape back out through the wound. For fairly large wounds, as air passes back and forth through the open wound it will create a sucking noise. The collapse of the lung on the injured side reduces the volume of air that flows into the lung, and compromises the patient's ability to oxygenate the blood and remove carbon dioxide.
- A closed pneumothorax involves an intact chest wall. The trauma could be the result of the lung bursting, or a rib fracture resulting in a lung injury that allows air to leak into the pleural space. As air leaks into the pleural space, the chest wall is no longer able to pull on the surface of the lung during inspiration, and the lung has a tendency to collapse due to its elastic recoil with a similar reduction in oxygenation to an open pneumothorax.
- Tension pneumothorax. Either an open or a closed pneumothorax may develop into a Tension Pneumothorax which is one of the most rapidly deadly traumas encountered in the field. In a tension pneumothorax, the air that leaks in through the lung or the chest wall is prevented from traveling back out by a "flap" of tissue that behaves like a one way valve. Air continues to be pulled in through the work of respiration. As the pleural cavity continues to fill with air with no vent, it increases pressure on the lung until it has fully collapsed, impeding air exchange. As the pressure continues to build, the collapsed lung and intrapleural-free air begin to push on mediastinal structures, including the inferior vena cava (IVC), superior vena cava (SVC) and the heart. This impedes blood flow back into the right atrium of the heart, leading to cardiovascular collapse and rapid death if untreated.[8] The rate that air enters into the pleural space will determine how quickly the patient will be compromised. Stay vigilant with any patient in which you suspect a pneumothorax, as their condition can change rapidly.
Documentation[edit | edit source]
Documentation of treatment for penetrating chest trauma should be included in the Patient Care Report (PCR) in the form:
- "Arrived to find patient lying supine on street being assessed by FD for CC of GSW. Patient is conscious and track EMS upon approach. Patient is diaphoretic, tachypneic, and exhibits obvious respiratory distress. Patient is a 36 yo Male who was shot x1 in the chest by 9mm pistol during drive by shooting. Patient assessment reveals sucking chest wound to the right chest, midclavicular with no obvious exit wound, Asherman seal placed. Further assessment reveals tracheal deviation, JVD and absent lung sounds on the right with clear lung sounds on the left. Secondary assessment reveals no further visible injuries or bleeding. Patient placed in full spinal motion restriction per protocol and loaded into ambulance. Due to short transport time and prolonged ALS response time, patient transported code 3 to trauma center without ALS intercept. Patient placed on oxygen at 15 lpm via NRM. Patient denies lightheadedness, dizziness, HA, weakness, changes to vision/hearing. Patient reports no increase in work of breathing during transport. Patient monitored during transport. Turnover report given to ED trauma team, patient care transferred. "
Self Assessment[edit | edit source]
- Review and practice with the Penetrating Chest Injury worksheet until comfortable with the workflow.
- Test your knowledge with this quiz
Tips and Tricks[edit | edit source]
- A sucking chest wound is classified as such if it is greater than or equal to 2/3 the diameter of the trachea.[9]
- If the penetrating trauma involves an object which remains lodged into the patient, do not remove the object unless it prevents care from being administered. Instead, stabilize the object with bulky dressings and transport.
Additional Resources[edit | edit source]
TBD - extra videos to watch, links to other pages for more reading
References[edit | edit source]
- ↑ https://emsa.ca.gov/wp-content/uploads/sites/71/2017/07/Skills-Form-7.1.17.pdf
- ↑ CP: c-spine involvement
- ↑ CP: pneumothorax = death
- ↑ CP: last sign trach dev
- ↑ CP: tension pneumo leading to shock
- ↑ CP: pneumo in unresponsive
- ↑ CP: improvised chest seal
- ↑ CP: tension pneumo pathophys
- ↑ CP: definition