NREMT Skillset/Hemorrhage Control
| Part of | NREMT Skillset |
|---|---|
| Subskill of | Circulation |
| Subskills | Scene Assessment Upon Arrival (PENMAN) Tourniquet Application Pressure Dressing Application Improvised Wound Packing Simulator |
| Equipment | Rolled Gauze Gauze Pads Elastic bandages Triangular Bandage CAT Tourniquet Wound packing simulator |
| Acting roles | EMR EMT emergency medical responder emergency medical technician paramedic |
| Pathologies | abrasion bleeding bruise burn contusion crepitus cyanosis cyanotic decomposition diaphoresis diaphoretic dislocation exsanguination hemoptysis hypotension hypothermia laceration lesion lividity pain pale tenderness |
| Body systems | circulatory system |
| Body parts | arm(s) chest feet hands head leg(s) lower extremities thorax upper extremities |
Hemorrhage Control is included in this California-based EMT program as it is required for skills verification for California Registration.[1]
Hemorrhage Control
Control of significant bleeding is a top priority during patient care as hemorrhage is the leading cause of preventable death in both civilian and military trauma.[2] "Circulation" including hemorrhage control and maintaining adequate perfusion is the C of the primary assessment ABC Airway/Breathing/Circulation mnemonic, and life-threatening bleeding should be addressed first - even before Airway and Breathing. Every second of uncontrolled bleeding worsens outcomes, and as an EMT in the prehospital setting, effective hemorrhage control is an essential skill.
The most commonly accepted and employed methods of hemorrhage control are:
- direct pressure,
- tourniquets, and
- wound packing with hemostatic agents.
In all cases, don't become so focused on the wound that you forget the rest of the patient. Stay alert to changes of the entire patient.
Direct Pressure
[edit | edit source]While it cannot control all bleeding, direct pressure will slow and even stop most bleeding if done correctly. To be effective, the first responder must make sure they are putting direct pressure on, and adequately collapsing, the primary vessel or vessels that the bleeding is coming from. Placing a palm on the area that is bleeding is seldom successful in large arterial bleeding because the pressure is too distributed. A smaller more concentrated pressure on the area where most of the bleeding is occurring is often more effective. For most wounds, start with direct pressure:
- Ensure that you as the responder have adequate PPE including gloves and eye protection.
- If there are deeply embedded objects protruding from the wound, DO NOT remove them. Employ bulky dressings to stabilize the object, and apply pressure around the object. Small objects such as gravel may be safely removed, but should not be the focus.
- Place a sterile gauze pad over the wound and place your gloved hand over the pad and apply direct pressure and hold it for several seconds.
- Use additional pads as needed if the first pads become soaked, and continue to apply pressure.
- For extremity wounds, check the distal pulse while holding pressure.
- If the wound shows signs that this direct pressure is effective at controlling the bleeding, after 3 minutes of manual pressure apply a pressure dressing, bandaging the gauze pad in place. Make sure to wrap the bandage tight enough to keep the bleeding under control but not limit circulation, and consider splinting wounded extremities to minimize disruption.
- For extremity wounds, recheck the distal pulse after bandaging the wound and if the pulse has disappeared, loosen the bandage a bit.
- Administer high flow oxygen and keep the patient warm, and transport immediately.
- Recheck both the pulse and the bandage for breakthrough bleeding at regular intervals during transport.
Once the bandage is applied, it should not be removed in the prehospital environment unless absolutely necessary. Removal of a dressing may do further damage to the affected area and increase the bleeding. Instead consider reapplying manual pressure or adding another elastic wrap bandage.
If the bleeding has not stopped with direct pressure, your next step depends on where the injury is:
- Extremities. Proceed to applying a tourniquet +/- wound packing.
- Axilla or groin. Tourniquets cannot be used, wound packing is the next option.
- Head and Neck. Continue with manual direct pressure only. Wounds of the neck aren't generally packed because of the risk for airway compromise, and care must be taken with head wounds in the presence of suspected skull fracture.[3]
- Chest/abdomen/pelvis. Occlusive dressings. Bleeding from the chest, abdomen, and pelvic area is often too deep to be reachable from the outside and should not be packed, use occlusive dressings and prioritize transport.[4]
All of these patients need rapid transport to definitive care.
Tourniquets
[edit | edit source]For extremity wounds in which direct pressure has been tried and has failed to control the bleeding, consider a tourniquet. Until recently, using tourniquets for prehospital hemorrhage control has been discouraged, however data from studying combat survival for trauma victims indicates that early use of tourniquets before the patient bleeds into shock increases survival by almost a factor of 10.[5] It is now recommended that EMTs carry tourniquets and apply them in the prehospital setting when extremity bleeding cannot be controlled with direct pressure.
The most common type of commercial tourniquet used in the field is a Combat Application Tourniquet (CAT) which consists of an adjustable strap, a tightening rod, called the windlass rod, clips for retaining the rod once tightened, and a strap to retain the rod in the clips.
To apply a Combat Application Tourniquet (CAT):
- DO NOT remove the gauze pads over the wound
- Place the tourniquet on the limb a minimum of 2" above the level of the bleeding (never over a joint) and fasten to itself tightly enough that 3 fingers cannot be slipped between the tourniquet and the limb.
- Use the windlass rod and twist to tighten until the bleeding stops and the distal pulse disappears. This should not take more than 3 turns, however it is critical that you apply the tourniquet with the aim of stopping the bleeding, not just slowing it down.
- Clip the windlass rod in place, and restrain with the strap.
- Write the time of application down on the tourniquet and record in the patient care report
- If bleeding has not been controlled with adequate tightening of the tourniquet, consider applying a second tourniquet next to the first.
- Transport immediately. When it has had a tourniquet applied, the limb has a limited amount of time to survive and needs to reach definitive care quickly.
If a commercial (CAT) tourniquet is not available, use an improvised tourniquet, for which you will need 3 things:
- Material - a band of some sort to wrap around the extremity
- Windlass - rigid object to twist the material (hand tightening is ineffective)
- Securing mechanism - something to keep the windlass from unwinding and loosening the tourniquet (Depending on the source of the material, this is optional as some materials may be wrapped around the windlass to prevent unwinding)
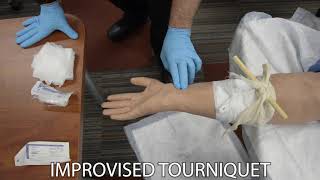
One of the more common improvised tourniquets is triangular bandage folded into a cravat, with a piece of wood or plastic used as a windlass to tighten it, and the tail ends are used to secure the windlass. With any tourniquet, use the same application steps above and be sure to document the time of application.
Complications. The most prevalent and serious complication of a tourniquet that has been poorly applied or left on for an extended period is Compartment syndrome. When circulation is interrupted for a prolonged period it leads to tissue swelling and cellular rupture. This swelling creates increased pressure on the blood vessels, muscle, and nerves inside a sheath of non-compliant fascia within the extremity (the "compartment"). The increasing pressure can become a run away cycle even after circulation is restored as more swelling makes the perfusion worse which increases the ischemia and swelling. If this process is not corrected, it can lead to permanent damage and possible amputation of the affected area.
There is an outdated practice of periodically loosening a tourniquet to allow circulation to enter back into the limb. This has not been shown to have clinical benefit, and is not recommended.[6]
Minimizing the time to definitive care is the most effective way to avoid complications from tourniquets.
Wound Packing
[edit | edit source]Using direct pressure and tourniquets on extremity bleeding is relatively straightforward for EMS providers. More challenging wounds to manage, however, are those in the junctional areas such as the groin and the axilla where tourniquets can't be used, or in the upper thigh where tourniquets are less effective. The bleeding in these locations is often deeper and maintaining adequate external pressure can be difficult or impossible, however wound packing techniques can often help.
Packing Technique:
- Stop the bleed. Apply direct pressure to the wound, use a gloved hand, and/or gauze, or clean cloth. Depending on the location of the wound, you can use your elbow or knee to apply the pressure while you set out supplies. Maintain pressure throughout the packing process.
- Choose your packing. Gauze impregnated with hemostatic agents is preferable for wound packing, but plain rolled gauze may also be used when hemostatic gauze is not available. There are many choices available, so review your County EMS Guidelines when purchasing material.
- Insert gauze. Start unrolling the gauze and inserting it deeply into the wound using an alternating finger technique. Feed the gauze in continuously in a uniform fashion and push each new portion in deeply and firmly as this allows you to maintain pressure while packing the wound. Do not put lumps of gauze into the wound as this will allow pockets to form, decreasing effectiveness.
- Over pack. Wound packing needs to be assertive and deliberate. Do not be shy when packing the wound. The general rule is: "Pack gauze in until there isn't any more room in the wound, and then pack in some more". Once the wound is packed, hold pressure for the wound for 3 minutes if the situation allows.
- Repack. (only if necessary). If you are using hemostatic gauze, and it has not managed to control the bleeding, the manufacturers of hemostatic gauze recommend removing the original packing and replacing it with fresh gauze packing.[7] The theory behind this is the first packing is not applying sufficient pressure to the vessel. Before doing this ensure that you have truly "over packed" from step 5.
Once wound packing has controlled the bleeding, manage any other life threats and transport immediately.
Documentation
[edit | edit source]Documentation of Hemorrhage control should be included in the Patient Care Report (PCR) in the form:
- Wounds found and treatments provided should be documented. Example: "Assessment reveals actively bleeding 2.5 cm laceration to right forearm and hemostatic abrasion to the right temple. Forearm injury bleeding controlled with direct pressure and dressing."
- Where the tourniquet was placed, type of tourniquet applied, time of application, patient response, and CSM reevaluation are all indicated. Example: "CAT tourniquet applied to right upper extremity 4 inches proximal to the elbow at 0945 to termination of blood flow. Distal circulation absent, sensation and motor functions intact."
- Document the NUMBER of gauze rolls when packing a wound. This gives the surgeon a definitive number of rolls that need to be removed. Example: "5x combat gauze rolls packed into medial thigh wound and secured with pressure dressing. Reevaluation does not find visible signs of active bleeding."
Self Assessment
[edit | edit source]- Practice with the Bleeding Control and Shock Management skills sheet until you achieve smooth workflow.
- Practice with CAT Tourniquet, Wound Packing, and Pressure Dressing skill sheets
- Test your knowledge with this quiz
- Practice with a hemorrhage control improvised wound packing simulator
Tips and Tricks
[edit | edit source]- PHTLS, one of several advanced trauma treatment programs, changes the normal ABCDE primary assessment to include X (eXsanguinating hemorrhage) at the beginning. This XABCDE method places importance on the initial identification and management of life threatening bleeds.
- If an improvised tourniquet is needed, make sure to choose a medium that is not too dynamic (does not stretch) and that is not too thin. The aim of a tourniquet is to compress the underlying vasculature enough to stop blood flow without causing additional trauma. If a thin, static medium like a shoelace is used, there is an increased chance of secondary injury due to the massive pressure the medium will cause on the underlying tissue. Although such a tourniquet is unlikely to "cut" into the flesh, it may cause vascular damage that otherwise would have been avoidable and can complicate treatment in the hospital.
- Blood pressure cuffs make useful improvised tourniquets if they are available and not needed to take a blood pressure. By definition, a blood pressure cuff should be able to arrest arterial blood flow without undue tissue damage.
- Tourniquets by design reduce blood flow distally. As the distal tissues become more hypoxic, cellular death may occur causing a release of intracellular components. Myoglobin and potassium are important intracellular components that may cause a worsening of the patient condition if a tourniquet is removed without sufficient medical interventions (such as one would find in a hospital). Negative side effects from tourniquets may not present for 1-3 hours in some cases, but around the 6 hour mark, there is a high likelihood that amputation may be indicated.[8]
- Hemorrhage control, especially tourniquets and wound packing, can be incredibly painful; be ready for your patient, if they are conscious, to express this.
- When performing ANY intervention that has the possibility of impeding blood flow (spinal motion restriction, wound care, cervical collar, etc.) make sure to check CSM before and after the intervention. Tourniquet application should be the only intervention where there is a LOSS of pulse; pressure dressings that cause a loss of distal pulses are no longer pressure dressings.
Additional Resources
[edit | edit source]- Compartment syndrome may be treated in the hospital with a fasciotomy.
References
[edit | edit source]- ↑ https://emsa.ca.gov/wp-content/uploads/sites/71/2017/07/Skills-Form-7.1.17.pdf
- ↑ CP: bleeding preventable death
- ↑ CP: head/neck hemorrhage
- ↑ CP: occlusives for chest/abdomen/pelvis
- ↑ CP: factor of 10
- ↑ CP: TQ loosening
- ↑ CP: recommendation to repack
- ↑ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2660095/
| Authors | GSTC |
|---|---|
| License | CC-BY-SA-4.0 |
| Cite as | GSTC (2020–2025). "NREMT Skillset/Hemorrhage Control". Appropedia. Retrieved June 4, 2026. |