NREMT Skillset/Back Assessment in Trauma
| Subskill of | Spinal Immobilization Adult |
|---|---|
| Acting roles | EMR emergency medical responder EMT emergency medical technician paramedic |
| Pathologies | Broken spine (potential) |
| Body systems | skeletal system nervous system |
| Body parts | thorax spine |
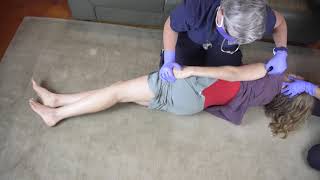
When assessing a trauma patient, assessment of the back and abdomen are the most common areas either missed or incorrectly performed. Assessment of the back follows the rules of trauma assessment; look for DCAPBTLS and any "abnormal" findings. Remember that there are spinal deformities that can be normal for a patient such as scoliosis and kyphosis. If your patient is lying prone, a back assessment may be quickly performed and a backboard (if one is being used) may be placed prior to log-rolling the patient.
Spinal assessment of the back covers the thoracic, lumbar, and sacral aspects of the spine. The cervical spine is commonly assessed during a back assessment as well, despite being part of a complete neck assessment. To perform a spinal assessment, place fingers on or just lateral to the bony prominences of the vertebrae and press inwards down the patient's back, assessing for tenderness, pain, or abnormal changes in sensation as you move. The spinal column should not have any significant step offs in a healthy patient. Remember that spinal tenderness refers to the tenderness found through this assessment; many patients who have musculoskeletal back injuries may exhibit pain or tenderness laterally to the spine but not of the spine itself.
Assessment of the back is particularly important in patients who have experienced penetrating trauma. Be sure to assess for exit wounds, which may not necessarily be found in a straight line from the entry wound. Presence or absence of exit wounds should be noted in the PCR and delivered to the trauma team or receiving caregiver on scene.
Self Assessment
[edit | edit source]- Test your knowledge with this quiz.
| Authors | GSTC |
|---|---|
| License | CC-BY-SA-4.0 |
| Cite as | GSTC (2020–2025). "NREMT Skillset/Back Assessment in Trauma". Appropedia. Retrieved May 31, 2026. |