This module allows medical officers, junior orthopedic surgery residents, and surgeons who are not orthopedic specialists to become confident and competent in irrigation and debridement, powered and manual drilling, positioning and correctly inserting Schanz screws, and constructing the uniplanar external fixator frame as part of external fixation procedures for open tibial shaft fractures performed in regions without specialist coverage. To maximize patient safety, this module teaches learners to use a powered drill to insert self-drilling Schanz screws through the near cortex and then manually advance Schanz screws into the far cortex to avoid plunging.
Self-Assessment Framework[edit | edit source]
After the reduced fracture has been stabilized with the uniplanar external fixator, please follow the 6 steps below, use a cellphone to take 5 post-operative photos ("digital X-rays"), and fill out the printed Training Logbook.
1. Take an anterior view photo with a ruler in the image to provide scale.
2. Visually inspect the tibial shaft and confirm that the alignment is within acceptable parameters:
- Bone apposition > 50%
- Rotation < 10 degrees
- Angulation < 10 degrees in the coronal plane
3. Use a ruler to measure the distance of the two near Schanz screws from the fracture line:
- Two near Schanz screws were placed at least 2.0 cm (a finger breadth) from the fracture line
4. Visually inspect the fracture line to confirm that the reduction is adequate:
- length discrepancy ≤ 2 cm shortening
- no distraction (lengthening)
- Take a medial view photo.
- Verify the far Schanz screw in the proximal fragment was inserted medial or distal to the tibial tuberosity.
- Confirm all four Schanz screws were inserted medial to the anterior tibial crest.
1. Take a lateral view photo.
2. Verify that all four Schanz screws did not perforate the far cortex.
3. Visually inspect the tibial crest to confirm that the alignment is within acceptable parameters:
- Bone apposition > 50%
- Rotation < 10 degrees
- Angulation < 10 degrees in the saggital plane
- Remove the rods and clamps but leave the four Schanz screws in the distal and proximal fragments.
- Use scissors to cut the cellophane wrap overlying the fracture site to separate the two fragments.
- Remove each fragment from the vise clamp and place each fragment on a flat surface for inspection of the drill trajectory angles.
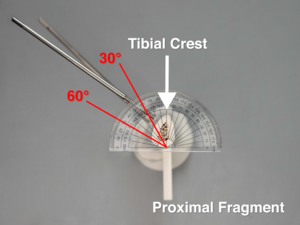
- Place a protractor on the cross-section of the proximal fragment as shown in the image. Line up the center vertical black line of the protractor with the center of the vise attachment.
- Take an overhead ("bird's eye view") photo of the cross-section of the proximal fragment to record the drill trajectory angles relative to the tibial crest. Check that the center vertical black line of the protractor is lined up with the center of the vise attachment in the overhead photo.
- For the proximal fragment, the drill trajectory angles of both Schanz screws should be identical and between 30°-60° relative to the tibial crest.
Subtract 90° from the protractor angle of each Schanz screw and calculate the absolute value of the drill trajectory angle.
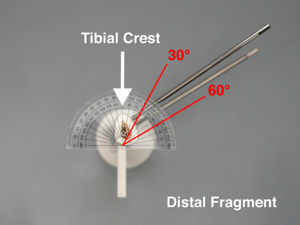
- Place a protractor on the cross-section of the distal fragment as shown in the image. Line up the center vertical black line of the protractor with the center of the vise attachment.
- Take an overhead ("bird's eye view") photo of the cross-section of the distal fragment to record the drill trajectory angles relative to the tibial crest. Check that the center vertical black line of the protractor is lined up with the center of the vise attachment in the overhead photo.
- For the distal fragment, the drill trajectory angles of both Schanz screws should be identical and between 30°-60° relative to the tibial crest.
- The drill trajectory angles of the proximal and distal fragments should be identical.
Subtract 90° from the protractor angle of each Schanz screw and calculate the absolute value of the drill trajectory angle.
Training Module Certificate of Completion[edit | edit source]
Once the self-assessment framework has been completed:
- Click the button above.
- Type in your name, download and print out a certificate of completion for this training module.
- Photograph your certificate on your cellphone as a backup and file the printed certificate in your training records.
Acknowledgements[edit | edit source]
This work is funded by a grant from the Intuitive Foundation. Any research, findings, conclusions, or recommendations expressed in this work are those of the author(s), and not of the Intuitive Foundation.