Cardiac Surgical Skills Training Module/Phase 1: Theoretical Knowledge/PDA Pathophysiology and Anatomy
| Part of | Cardiac Surgical Skills Training Module |
|---|
PDA Incidence
[edit | edit source]Almost 1% of all births are complicated by congenital heart disease. The reported incidence of PDA in term neonates is only 1 in 2,000 births, accounting for 5%–10% of all congenital heart disease. The incidence of PDA in preterm neonates is far greater, with reports ranging from 20%–60% depending on population and diagnostic criteria.
PDA Anatomy
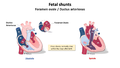
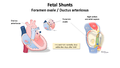
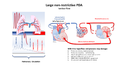
[edit | edit source]PDA is present during neonatal circulation as an essential while fetus in developing (during fetal development about 60% of the RV blood is diverted from the lungs through the ductus arteriousus). Usually closes within several hours to 3 days after birth, Closes in stages first constricts and then formation of connective tissue (can take up to 3 weeks). The precise mechanism of closure, is not completely understood but it is mediated by the release of vasoactive substances and also help by Oxygen (high Pao2).
Anatomic or Physiologic Problem
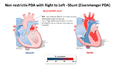
[edit | edit source]A vessel between the main pulmonary artery and descending thoracic aorta. Allowing blood to shunt from the aorta into the pulmonary artery due to the decreased PVR. The amount of left to right shunting depends on the size of the PDA- and the relative resistance of the systemic and pulmonary circulations. If it is big, it may lead to extensive aortic runoff, with low aortic diastolic pressures which can cause systemic organ hypo-perfusion.
Potential Stages of Disease
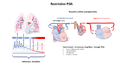
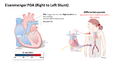
[edit | edit source]A large non-restrictive ductus with no other cardiac issues creates a left to right shunt with LA dilatation, LV volume overload and progressive heart failure. –if untreated a large PDA may lead to pulmonary arteriolar hypertension with the eventual development of right to left shunt and Eisenmenger physiology. High PVR may develop as early as 6 months of life resulting in supra-systemic pulmonary artery pressures.
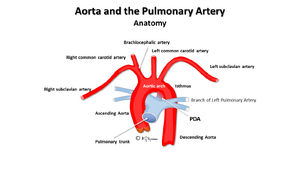
Aorta and the Pulmonary Artery
[edit | edit source]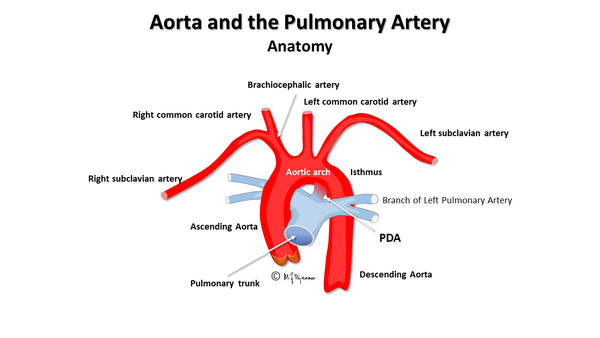
Fetal Shunts
[edit | edit source]Normal Physiology
[edit | edit source]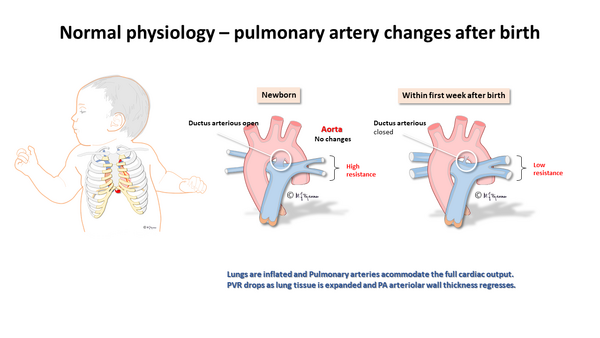
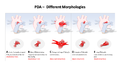
PDA Morphologies
[edit | edit source]PDA Pathophysiology
[edit | edit source]At birth the increased in PAO2 is the most important stimulus for the ductus arteriousis to constrict: typically occurs within 24 hours of birth, permanent closure of the ductus arteriousis occurs over the first few weeks after birth. In premature infants the ductal tissue is less reactive to oxygen, post ductal closure is less common. Left to Right shunting leading to an increased pulmonary blood flow (PVR is less than SVR, resulting in increased pulmonary blood flow). If restrictive, the amount of shunt is determined by the size of the defect.
Normal Heart with PDA
[edit | edit source]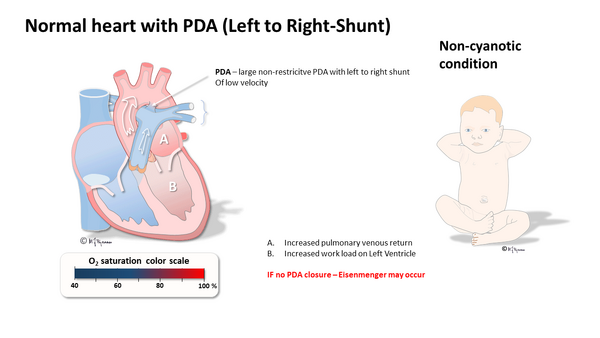
Eisenmenger PDA
[edit | edit source]Resources
[edit | edit source]| Authors | Owen Robinson |
|---|---|
| License | CC-BY-SA-4.0 |
| Organizations | Global Surgical Training Challenge |
| Cite as | Owen Robinson (2021–2025). "Cardiac Surgical Skills Training Module/Phase 1: Theoretical Knowledge/PDA Pathophysiology and Anatomy". Appropedia. Retrieved June 3, 2026. |