NREMT Skillset/Ventilation of an Intubated Patient
| Acting roles | EMT emergency medical technician paramedic |
|---|---|
| Pathologies | congenital hypoxia |
| Body systems | respiratory system |
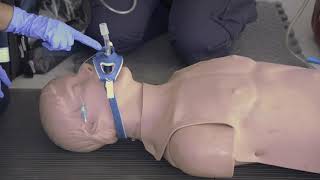
Ventilations of an intubated patient should take place every 6 seconds. This 6 second rule is true of any advanced airway which includes supraglottic airways such as a King Tube or Laryngeal Mask Airway (see below). Each ventilation should be delivered smoothly over 1-1.5 seconds and should produce adequate chest rise and fall. The entire bag does not need to be emptied, in fact doing so will often over ventilate the patient and lead to complications such as barotrauma.
Attach the BVM to the port at the proximal end of the advanced airway and hold it in place with opposing pressures. When ventilating, the head-tilt chin lift procedure may be used if ventilations need to be troubleshot, but an intubated patient does not require such a procedure to be adequately ventilated as the endotracheal tube has been passed into the trachea past most potential anatomical roadblocks.
Note the depth of the ETT when ventilations have been started and continually reassess that the depth has not changed, especially after any high motion procedure such as placing the patient on a backboard or stretcher or moving the patient to/from the ambulance. Any changes to the depth of the ETT should immediately be reported to the paramedic.
-
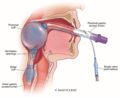
King Tube
-
Laryngeal Mask Airway
| Authors | GSTC |
|---|---|
| License | CC-BY-SA-4.0 |
| Cite as | GSTC (2020–2026). "NREMT Skillset/Ventilation of an Intubated Patient". Appropedia. Retrieved June 4, 2026. |