ALL-SAFE will allow surgeons in low-resource settings to become confident and competent in performing basic laparoscopy.
Why ALL-SAFE?[edit | edit source]
Laparoscopic surgery has become the standard technique of surgical care for many procedures. The general benefits of laparoscopy over open surgery are well-established and may be amplified in low-middle income countries where advances in infection rates, length of stay, and convalescence could translate into meaningful and scalable gains in health outcomes, economics, and healthcare utilization regionally and nationally.1
Laparoscopic skills have been shown to improve with simulation-based training.2,3 However, laparoscopic surgical training remains inaccessible and understudied in many low- and middle-income countries (LMICs) including Sub-Saharan Africa, resulting in its underutilization. Major barriers to laparoscopy in LMICs include a shortage of funding for equipment and training, a lack of local expertise or skills, and a hierarchical surgical culture in which faculty take priority in learning this technique over surgical trainees.4,5
The goal of ALL-SAFE is to overcome the educational barrier by teaching surgeons in the low resource setting to perform laparoscopy safely, confidently, and competently. We currently offer five modules on the laparoscopic management of: ectopic pregnancy, appendicitis, Meckel's diverticulum, penetrating thoracoabdominal trauma, and trocar placement. These particular pathologies were chosen because they are common worldwide and can be treated safely laparoscopically with significant benefit to the patient. Laparoscopic management of these common pathologies also convey a skillset that can be used more broadly in all basic laparoscopy.
ALL-SAFE’s content is designed for medical professionals who have completed, or are in the process of completing, their surgical training and know how to perform the open surgery equivalent of procedures taught on this site. This curriculum is designed to be used in the context of other laparoscopic surgical training activities.
The Goals of ALL-SAFE[edit | edit source]
- To improve the surgeons' confidence and competence in the laparoscopic management of basic surgical conditions
- To support the development of basic cognitive and technical skills required for the safe laparoscopic management of basic surgical conditions
- To provide surgeons with standardized educational content on the laparoscopic management of basic surgical conditions to assist in development of relevant clinical judgment
- To provide a formative assessment framework and objective quantifiable measures to assess knowledge, judgment, and manual skills in the laparoscopic management of basic surgical conditions
- To promote collaboration between countries of diverse resource levels to provide a low-cost, open source, portable educational and assessment framework to improve quality of surgical care
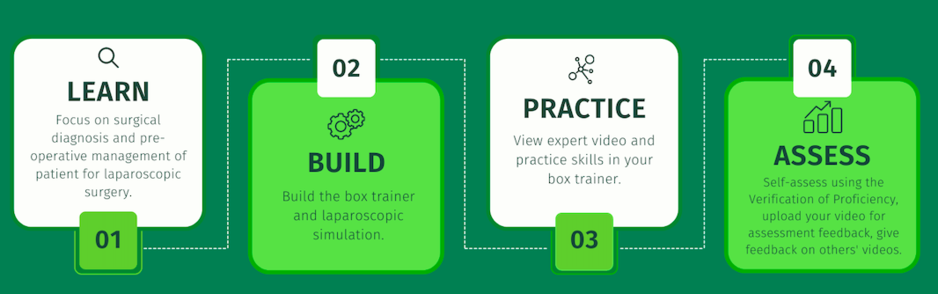
This course is organized into four components.
Learning Objectives[edit | edit source]
Our team has created a comprehensive list of learning objectives for our learners. Please see the document below on how our platform meets these specific learning objectives for our first module on ectopic pregnancy as a representative example.
Accessibility[edit | edit source]
While this course is available to any interested surgical learner, our target learner is the surgeon or surgical resident who is already comfortable performing open surgery. The entire module is available through open-source learning on the web through an online, freely accessible site. Users need an unique identifier that they obtain through email signup to track their own learning, but the generation and assignment of the unique identifier is automatic and instantaneous. The materials that are needed to build the box trainer and models are universally available. The only pieces of technology that the learner needs are a cellphone and a computer which are generally available and laparoscopic instruments which are available in the hospital setting.
- There are 3 ways to access our ALL-SAFE platform.
-
ALL-SAFE Platform DEMO, --for exploring and browsing--For Judges, please use this demo version. This demo course will allow you to freely navigate through the modules, repeat modules, and repeat quizzes. In addition, you will not be required to submit a video or review videos in order to complete the course. We have created this demo course so that you are able to see all our content on the native platform.
-
ALL-SAFE Platform for LEARNERS, --for learners to officially go through modules--
-
Appropedia Version, --for a surrogate descriptive experience-- Appropedia will provide a surrogate experience of our platform through screengrab videos and background information on our project and its projected scope. You will be able to see most cognitive and psychomotor components on Appropedia; however, a learner will not be able to do most assessments through Appropedia.
Innovation[edit | edit source]
- The learning content captured in a full clinical case
- The learner practices psychomotor skills in a box they can built themselves, performing actual technical components of the operation
- Box trainer utilizes a resource common to most – cellphone – for video capture
- Skills and techniques based on equipment and technology that would be available in low-resource setting
- ALL-SAFE is ready for immediate use
Collaborations and Funding[edit | edit source]
This effort is a collaboration of members from the Pan-African Academy of Christian Surgeons (PAACS), the College of Surgeons in East, Central, and Southern Africa (COSECSA), the University of Michigan, Southern Illinois University, Soddo Christian Hospital, Mbingo Baptist Hospital, and AIC Kijabe Hospital. Funding for this study has been provided by the Global Surgical Training Challenge.
- Collaborations and Funding
-
-
-
-
-
-
-
-
-
-
References[edit | edit source]
1) Rosenbaum AJ, Maine RG. Improving Access to Laparoscopy in Low-Resource Settings. Ann Glob Health. 85(1). doi:10.5334/aogh.2573
2) Sroka G, Feldman LS, Vassiliou MC, Kaneva PA, Fayez R, Fried GM. Fundamentals of laparoscopic surgery simulator training to proficiency improves laparoscopic performance in the operating room-a randomized controlled trial. Am J Surg. Jan 2010;199(1):115-20. doi:10.1016/j.amjsurg.2009.07.035
3) Korndorffer JR, Dunne JB, Sierra R, Stefanidis D, Touchard CL, Scott DJ. Simulator training for laparoscopic suturing using performance goals translates to the operating room. J Am Coll Surg. Jul 2005;201(1):23-9. doi:10.1016/j.jamcollsurg.2005.02.021
4) Choy I, Kitto S, Adu-Aryee N, Okrainec A. Barriers to the uptake of laparoscopic surgery in a lower-middle-income country. Surg Endosc. Nov 2013;27(11):4009-15. doi:10.1007/s00464-013-3019-z
5) Farrow NE, Commander SJ, Reed CR, et al. Laparoscopic experience and attitudes toward a low-cost laparoscopic system among surgeons in East, Central, and Southern Africa: a survey study. Surg Endosc. Dec 2021;35(12):6539-6548. doi:10.1007/s00464-020-08151-w
6). Sroka G, Feldman LS, Vassiliou MC, Kaneva PA, Fayez R, Fried GM. Fundamentals of Laparoscopic Surgery simulator training to proficiency improves laparoscopic performance in the operating room—a randomized controlled trial. The American Journal of Surgery. 2010;199(1):115-120. doi:10.1016/j.amjsurg.2009.07.035
7). Gheza F, Oginni FO, Crivellaro S, Masrur MA, Adisa AO. Affordable Laparoscopic Camera System (ALCS) Designed for Low- and Middle-Income Countries: A Feasibility Study. World J Surg. 2018;42(11):3501-3507. doi:10.1007/s00268-018-4657-z
8). Van Duren B, Boxel G. Use your phone to build a simple laparoscopic trainer. Journal of Minimal Access Surgery. 2014;J Minim Access Surg.:219–220. doi:10.4103/0972-9941.141534